The Affordable Care Act of 2010, or Obamacare, as the bill is colloquially known, reformed health care policy in the United States as we knew it. While the Act continues to be amended to this day, its overarching goal is to increase access to health insurance. In chapter two of Decoding Health Insurance, Lauren Jahnke writes, “[The ACA] attempts to fix many issues experienced in different parts of the healthcare system, including in the individual insurance market, Medicaid, and Medicare. It also offers new consumer protections and other programs.”
Affordable Care Act Status in 2021
After Congress passed the ACA along party lines, there have been about 70 attempts in the House, Senate, and most recently by Donald Trump’s administration, to defang and ultimately strike down Obamacare for good. But as of January 20, 2021, the ACA still stands. And with the party that spearheaded the bill in control of the executive and legislative branches of government, until at least 2022, there’s an expectation that in the immediate future, lawmakers will work to protect and bolster the Affordable Care Act.
Here are a few major ways the Affordable Care Act of 2010 transformed the health care system in the United States.
Ten essential health benefits
All plans in the marketplace are required to provide 10 essential health benefits. You can get details on all 10 at Healthcare.gov, but they include outpatient care, emergency health care, surgery and overnight hospitalizations, maternity and newborn care, mental health, prescription drugs, preventive and wellness services, and laboratory services. We explain a few ACA benefits here.
Establish marketplaces
Marketplaces were established so that people can compare health care plans and prices in one place. States were given the option to create their own exchanges. The Kaiser Family Foundation recently compiled a report detailing marketplace types by state. In 2021, 15 states operate their own individual health insurance marketplaces; 6 states rely on a platform developed by the federal government; and citizens of 30 states can purchase health insurance from the marketplace developed and maintained by the federal government.
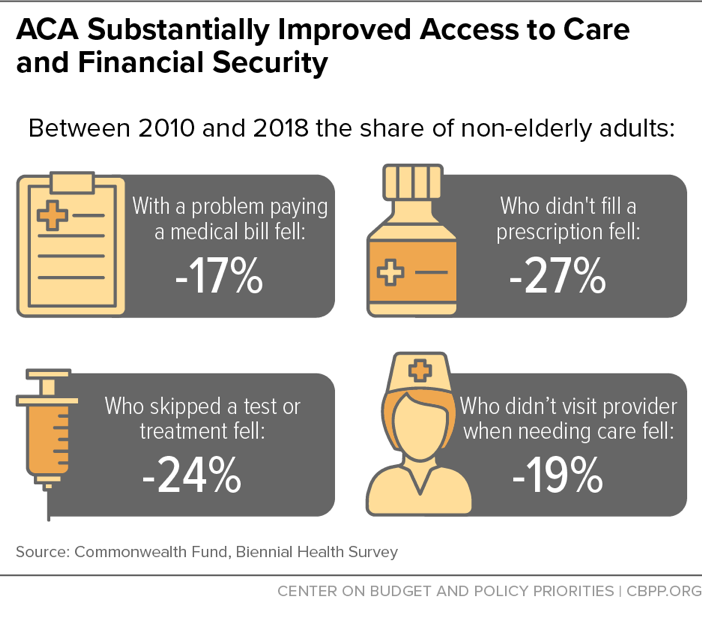
Tax subsidies
Subsidies, also known as tax credits, were created to help people pay for health insurance. The way subsidies were set up is that they reduce the cost of monthly premiums and charge customers on a sliding scale, based on income.
Preexisting conditions
The law required insurers to cover preexisting conditions. Prior to the ACA, customers could be denied coverage or get kicked off their health insurance plan for conditions like pregnancy, diabetes, heart disease, and even obesity. In other words, anyone could be disqualified from a health plan or coverage for almost any reason. According to the Centers for Medicare & Medicaid Services, “50 to 129 million (19 to 50 percent of) non-elderly Americans have some type of preexisting health condition.” Starting in 2014, insurance companies could no longer deny coverage or charge significantly higher premiums if a customer has a preexisting condition, including a life-threatening illness or chronic condition.

Source: Vox.com
Preventive care
Insurers were required to provide in-network preventive care, such as immunizations, mammograms, and cholesterol tests, at no additional cost to patients.
Individual mandate
The individual mandate was a penalty charged to anyone (not including those who qualified for an exemption) who did not have health insurance. It was eventually repealed — or, technically, the penalty was reduced to $0. As of November 2020, five states and Washington D.C. had reinstated an individual mandate, according to eHealth. Some believe striking down the mandate was a bad-faith effort by conservative legislators to abolish the entire act. But that never happened. After the individual mandate was eliminated on a federal level, Sarah Kliff wrote in the New York Times, “Participation in Obamacare marketplaces has decreased slightly, to 11.4 million this year from 12.2 million in 2017. But it hasn’t plummeted or shown any signs of a “death spiral,” in which only sick patients purchase coverage and premiums become unaffordable.” According to the Kaiser Family Foundation, the individual mandate was a very minor reason why people opted for or against enrolling in Obamacare.

Source: cnn.com
The last time the Senate voted to repeal the ACA, the decision hinged on Senator John McCain. His thumb’s-down vote, with Senate Majority Leader Mitch McConnell standing just a few feet away, is an iconic image in the country’s collective memory. While President Trump promised to repeal and replace Obamacare, neither he nor any Republican ever presented a comprehensive health care plan to the American people. In 2017, according to Politico, Trump did admit, “Nobody knew that health care could be so complicated.”

Coverage for kids
Children could stay on their parents’ health care plans until age 26. There were also provisions for kids in the foster care system. Prior to the ACA, kids aged-out of their parents’ plans by age 19 or 22, depending on their student status. The first year ACA went into effect, roughly 7.8 million young people were able to stay on their parents’ health insurance plans, according to NBCNews.com.
No annual or lifetime caps
Before Obamacare, insurance companies could cut patients off if they hit some arbitrary dollar limit on their plan. Insurers could ding customers on two fronts: by implementing a lifetime dollar limit and an annual dollar limit.
Expand Medicaid eligibility
The ACA gave states the option to expand Medicaid eligibility to adults under the age of 65. Non-elderly adults whose income was at or below 133% of the poverty line could qualify for Medicaid. Since states run Medicaid programs, a judge ruled that states could determine whether or not to expand their Medicaid programs. The 12 states that have opted out of the program have left millions of financially insecure Americans without health care coverage, according to the Kaiser Family Foundation.
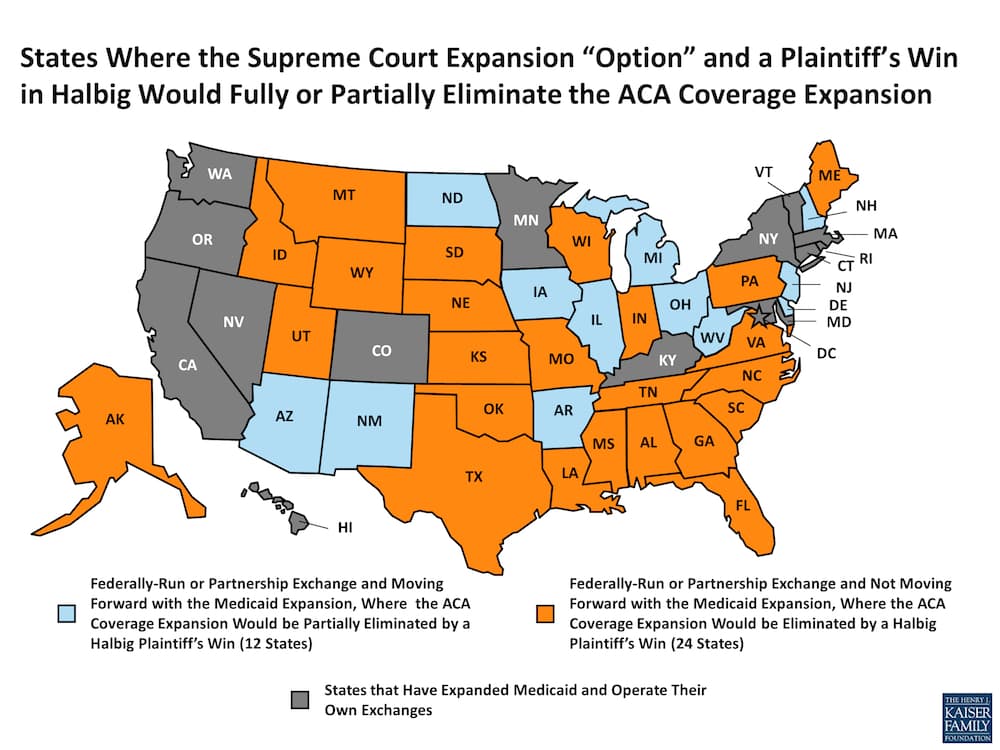
Employer provisions
Small businesses can obtain health insurance through the Small Business Health Options Program (SHOP) marketplace. Also, certain businesses with fewer than 25 full-time employees that offer health insurance may qualify for a tax credit. In a study titled, “The Affordable Care Act’s Impact on Small Business,” published in 2018, David Chase and John Arensmeyer wrote, “[T]he uninsured rate for small-business employees fell by almost 10 percentage points post-ACA.” The researchers also stated that the law helped “stabilize health costs for many small businesses that provide coverage, with the rate of small-business premium increases falling by half following implementation of the law.”
Why is Health Care Controversial?
So why has the ACA been so controversial for so long? This question doesn’t really have a simple, pithy answer. But conservatives say they don’t like the added tax costs and as far as the health care industry is concerned, implementing new policies are time consuming and expensive. Or course, the private health insurance industry didn’t like the competition, not to mention the many ways the law prevented them from cushioning their profits even more. So they spent loads of money on lobbyists, which put dollars in lawmakers’ pockets. So maybe the GOP’s problem with Obamacare didn’t really have anything to do with taxes after all. It’s hard to say. According to Jahnke, “The only issue is that adding more benefits and protections inevitably causes the price of health insurance to go up as insurance companies pay for more health care, so it’s a double-edged sword that is very difficult to adequately resolve.”
Read Decoding Health Insurance
To better understand the U.S. health care system, check out Decoding Health Insurance and the Alternatives: Options, Issues, and Tips for Saving Money. You’ll find informative, nonpartisan information and tips for buying health insurance and saving money on health care, whether or not you have coverage.
